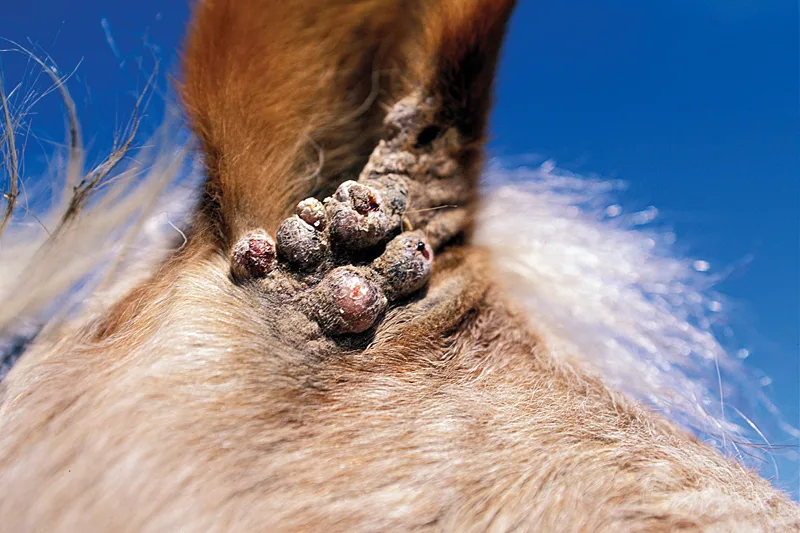
These benign but bothersome tumors are as individual as the array of potential treatments
They’re the most common type of skin tumor in horses, and they’re usually not all that alarming—but although they’re categorized as benign, sarcoids have plenty of troublesome potential.
The thing about sarcoids is, they’re devilishly difficult to defeat. Although they seem to have a common cause—a virus called bovine papilloma, which causes warts in cows—they are masters of disguise, taking any number of different forms and casually defying any kind of easy cure.
Not all sarcoids need curing, of course. When they appear in non-troublesome places on the horse’s skin, and just sit there doing nothing in particular, they are better left alone. But sarcoids that sprout in more troublesome locations—such as the eyelid, the ear, or any spot where tack or equipment might rub or chafe—can cause more than their fair share of grief and need to be dealt with.
Research has been done on sarcoid tumors in horses and just as much done on methods of attacking them. Despite a growing list of treatment options, no one method has leapt out at the scientific community as “The Answer.” So sarcoids present a unique challenge to the clinician: which treatment approach to use on which sarcoid?
Before we delve into the array of weapons at our disposal, let’s get to know the enemy a little better.
Up Close And Personal
The typical equine sarcoid is found on the skin surface and closely resembles a wart. Some are small and flat, with a crusty surface or a normal skin covering; this type (sometimes called a verrucous sarcoid) grows slowly and may remain static for years at a time, or may even spontaneously disappear.
Others, sometimes called fibroblastic sarcoids, are more aggressive and invasive; they have a raised, bumpy surface, may bleed or ooze serum if they’re bumped or rubbed, and can rapidly proliferate into large, angry-looking masses.
Sarcoids can appear anywhere on the skin surface, and horses of any age, breed or color are susceptible. The areas most frequently affected include the skin of the head (especially the mouth, eyelids and ears), the legs, tailhead, the underside of the barrel, and anywhere with thin skin, limited or no haircover and a tendency to sweat. Wound sites, and former wound sites, are another vulnerable area.
Sarcoids can appear singly, but often they’ll show up in several locations on a horse, a characteristic that supports the now widely accepted hypothesis that most, if not all, sarcoids have a common infectious raison d’etre in the bovine papilloma virus. BPV causes ordinary warts in cattle—non-malignant and pretty harmless—but in horses, which are not the virus’ natural hosts, BPV seems to stimulate something nastier.
Researchers including Elizabeth Carr, DVM, Dipl. ACVIM, an associate professor at Michigan State University, suspect that horses are a “dead-end host” for BPV. The virus goes through an altered lifecycle in equine cells, never managing to replicate and shed virus particles as it does in cattle.
As a result, sarcoids don’t seem to be contagious from horse to horse. It’s more likely that horses somehow contract the virus from the environment (not even necessarily from being in contact with a wart-infested cow). Flies are one likely suspect, since sarcoids tend to sprout where flies tend to congregate, such as the eyes, the groin area and wherever there is an open wound.
ADVERTISEMENT
Regardless of how it gets there, it’s likely that the presence of BPV is the most significant initiating event in sarcoid development.
Is a sarcoid a tumor, then, or is it an infection?
The answer seems to be: both. Despite its infectious origins, however, the search for an effective vaccine has so far proven elusive.
Sarcoids are tumors of the fibroblasts, cells that help make up the structure of the skin. Rarely, sarcoids do develop in the tissues immediately beneath the skin, but they do not spread to the internal organs. A typical sarcoid is slow growing or static and has benign clinical behavior, although occasionally tumor growth does get aggressive (and very rarely, malignant).
Despite their benign nature, [sarcoids have a propensity to multiply, and individual lesions may enlarge slowly or rapidly.] When these lesions become ulcerated or cracked, and ooze blood or serum, they can become debilitating (and attract flies, which may help spread the disease). And in certain locations, such as the eyelids and over joints and coronary bands, they can become extremely difficult to treat.
Derek Knottenbelt, OBE, BVM&S, DVMS, Dipl. ECEIM, MRCVS of the University of Liverpool’s Department of Veterinary Clinical Sciences, expanded the number of sarcoid categories to six:
- Occult – circular patches of hair loss with a gray, scaly surface, which can look very much like ringworm; common on the face.
- Verrucose – gray and scaly but extending deeper than occult sarcoids and more irregular in outline (these often occur in multiples).
- Nodular – raised nodules up to 5 cm in diameter, commonly occurring around the eyelids and the groin, or anywhere under thin and hairless skin.
- Fibroblastic – aggressive, fleshy masses that often begin as a complication of a skin wound and grow rapidly, becoming ulcerated or developing a “stalk” of tissue; these can be extremely invasive.
- Mixed – showing qualities of two or more of the above types of sarcoids, often in a “colony.”
- Malevolent – the most aggressive type, commonly found on the face or around the elbow. It spreads through the skin and along the lymphatic system, with secondary ulcerated lesions. Fortunately, very rare.
Because biopsies are risky—the act of pinching out even a tiny tissue sample from a sarcoid tumor is often enough to “aggravate” it and trigger aggressive new growth—visual identification often suffices for sarcoids, though there are at least half a dozen other conditions that can produce similar-looking lesions.
And identification is only half the battle. The other half is deciding whether you want to try to treat the lesion or lesions and choosing the treatment most likely to a) do more good than harm, b) not cause the horse unnecessary pain or stress, and c) be within the owner’s budget and the treating veterinarian’s capabilities and comfort zone.
Talking Treatment
“Whether you pursue treatment depends on the size of the tumor and its location, but once they get past a certain size, or the tumor changes to malignancy, you may not have the option of treating them anymore. For most sarcoids, it’s a good idea to explore treatment early on,” said Carr.
But which treatment?
There are a bewildering number of options, all with pros and cons and variable success rates. Part of the difficulty is that no two sarcoids are alike in how they respond to treatment. Despite decades of research, there’s no one single treatment with a standout success rate in curing sarcoid tumors; often, control is the best you can hope for.
“The choice of treatment is governed by a number of factors,” said Knottenbelt. “The fact that there are some 40 treatments reported simply means that no one is universally successful. It’s also complicated by the fact that individual vets have individual treatments they have success with, and by the fact that many publications have reported treatments with very small samples sizes. Three to 20 cases (for a particular modality) are not nearly good enough for any meaningful outcome assessment.
ADVERTISEMENT
“Some treatments work better or worse in some anatomic locations and on some individual horses; others don’t,” he added. “The gold standard is radiation, which carries a 95 percent success rate, but which has severe difficulties both with cost, logistics (fewer than five hospitals in North America are capable of doing radiation therapy on horses), and the fact that it’s only applicable to smaller lesions.”
So, with radiation therapy ruled out for most of us, that leaves:
- Surgical excision, either by scalpel or laser.
- Cryonecrosis (freezing with liquid nitrogen).
- Ligation (tying off a protruding tumor so as to constrict the blood supply).
- Chemotherapy, usually in the form of drugs injected locally into the tumor.
- BCG (Bacillus Calmette-Gurein) injections, a human vaccine for tuberculosis that has proven particularly useful as an immune stimulant, in treating sarcoids around the eye or eyelid, injected into the lesion.
- Topical anti-cancer drugs, often borrowed from human medicine.
- Photodynamic therapy – chemicals that are injected into the lesion, then exposed to a specific wavelength of light to “activate” them.
Frequently, veterinarians will use more than one of these methods in combination, depending on the size and location of the sarcoid and whether it’s benign or rapidly growing.
Carr said, “For me, the size, location and type of tumor all have a bearing on which treatment I suggest. And there are also certain methods with which I have a comfort level. As a rule, bigger tumors are harder to cure, so I prefer to start when they’re smaller and more manageable. I also get much more aggressive with treatment if the tumor is actively growing.
“But the truth is there is no magic bullet yet, and the sarcoid’s viral nature may be part of the reason,” she continued. “We’re finding that even the normal skin margins around a tumor may harbor latent bovine papillomavirus, which means there’s great difficulty in completely eradicating it, and a higher risk of the tumor recurring.”
The virus is so resilient, in fact, that it has so far repelled every effort to develop an effective vaccine against it.
Carr, who has devoted much research into vaccine development, said, “There have been some promising results, but there is still no commercially available vaccine. The formulations we’ve come up with thus far may decrease the size or virulence of a tumor, but they don’t cure it.”
More promising, she said, is a drug called imiquimod (aka Aldara), a topical cream used to treat human papillomavirus lesions and some types of skin cancer. Initial studies at the University of Minnesota have suggested that imiquimod is potentially an excellent treatment for horses.
“It’s looking pretty useful,” Carr said. “The snag right now is that it’s marketed for humans in tiny packages, and you have to apply it about three times a week, so it can get fairly expensive.”
Another “really effective drug,” according to Carr, is cisplatin, a form of chemotherapy that, like all of its ilk, has pros and cons.
“The injectable form of cisplatin is very oily and hard to work with, and the treatment has to be repeated regularly,” she explained. “So now we’re moving to these biodegradable beads that contain cisplatin. They’re implanted in the tumor margins about one centimeter apart, and they slowly biodegrade and release the drug over the course of 30 days.
“Delivered this way, cisplatin has about an 80 percent success rate, and it’s good for larger tumors, unlike most of the other treatment methods. Even if you’re implanting a large number of the beads, there’s not enough systemic effect to be risky to the horse, but on the down side, the beads are really fragile and easy to crush when you’re implanting them, so it’s a little tricky,” she added.
Regardless of the approach you use to tackle your horse’s sarcoids, it’s important to be realistic about the results. Sarcoids are tenacious and frequently recur, sometimes within weeks of their apparent eradication. Or the treatment may only succeed in reducing the tumors’ size, number or severity. Cures are rare; control is a more practical goal—at least until someone develops that elusive magic bullet.
If you enjoyed this article and would like to read more like it, consider subscribing. “Sarcoid Solutions” ran in the Nov. 12, 2010 issue. Check out the table of contents to see what great stories are in the magazine this week.