A mare comes in from the field one afternoon with an eye that is red, irritated and tearing. Her owners chalk it up to flies and buy a fly mask. While the mask helps keep insects away from her eyes, the mare continues to suffer with painfully puffy, weepy eyes. By the end of the week, they notice that the eye looks cloudy and the mare is reluctant to come out of her stall into the sunlight. Alarmed, they call the veterinarian who concludes the examination with a worrisome diagnosis: uveitis, which is more formally known as periodic ophthalmia, or ERU, for equine recurrent uveitis.
The mare’s red and weepy eye is treatable with atropine to help dilate the pupil and reduce the discomfort, followed by antibiotic eye drops and anti-inflammatory drugs. However, uveitis, commonly known as “moon blindness,” often recurs.
ERU Explained
Moon blindness is the most common cause of blindness in horses and mules. It affects up to 12 percent of horses worldwide and about 25 percent of Appaloosas (Quarter Horses being the next most vulnerable breed). The symptoms include:
- tearing
- cloudiness on the surface of the eye
- a type of scarring called butterfly lesions
- redness and puffiness around the eye
- muscle spasms which keep the eye tightly closed
- rubbing the eye
- head shaking
- loss of balance or stumbling
- pain and irritability
- excessive squinting and blinking
- a sensitivity to bright light (photophobia)
- constricted pupils
In the worst cases, symptoms can escalate to include:
- detachment of the retina
- calcification of the cornea
- cataracts
- atrophy of the eye
- eventual blindness in one or both eyes
The clinical signs may reappear every few weeks or months once a horse has suffered an initial episode. Each flare-up can last up to a couple of weeks, and with each succeeding episode, the damage accumulates.
Aggressive treatment as soon as symptoms are noticed can minimize the detrimental effects, but many horses still gradually lose their vision.
The disease usually affects one eye at a time, but it’s not uncommon for the second eye to also develop symptoms, sometimes turning a horse completely blind.
Ancient Root Of The Problem
According to equine ophthalmologist Dennis Brooks, DVM, Ph.D., of the University of Florida in Gainesville, moon blindness has been plaguing horses for millennia.
“There are medical historians who think that moon blindness is the oldest recorded disease, older even than recorded human disease,” said Brooks. “It’s an old, old disease, but only in the last 10 years or so have we begun to understand what its causes are.”
Bacterial, fungal, viral and parasitic infections have all been implicated in ERU, with a bacterial disease called leptospirosis being one of the most common triggers. Horses can contract leptospirosis through exposure to contaminated feed or water, and the bacteria can also linger for years in soil where cattle have lived or where springtime flooding has occurred. ERU that develops in the wake of a leptospirosis infection may take a year or two to surface, long after the infection has gone.
Another possible cause of ERU is a parasitic infection called onchocerciasis. Horses contract the parasite, Onchocerca cervicalis, when they’re bitten by Culicoides flies, which are tiny midges. The parasitic larvae, called microfilariae, create weeping sores on the withers, the underside of the mane and the midline of the abdomen, and when they get in the tissues of the eye, they can cause intense irritation.
Ironically, broad-spectrum dewormers such as ivermectin, normally considered a benefit to equine health, can sometimes set off uveitis when they kill off large quantities of microfilariae in the eyes of an infected horse. This is because the immune system reacts more violently to dead microfilariae than live ones.
ERU can also take hold thanks to any of a number of common viral infections, such as influenza and equine herpes virus. Trauma to the eye can begin the destructive cascade as well. Corneal ulcers, intraocular surgery or any blunt or invasive force sustained by the eye can make the tissues vulnerable to ERU, as can allergies to certain pollens.
Said Brooks, “[ERU is] probably an immune-mediated disease. Infection can start it or trauma can start it. Something starts it, and whatever that initiating factor is, it heals, and you’re left with the autoimmune disease.”
ADVERTISEMENT
In an autoimmune disease, the horse’s own immune system mounts an inappropriate inflammatory response. In the case of ERU, it’s against proteins in the eye. The T-lymphocyte response launched by the immune system triggers intense inflam-mation in the eye and sets the stage for long-term damage.
“What happens in these horses is that they get little collections of T-lymphocytes within their eyes. This is why the disease gets worse, and it keeps coming back, and it goes through these cycles. These lymphocytes are in little follicles, little structures which aren’t supposed to be [in the eye]. It took us a long time to figure that out,” Brooks said.
“It doesn’t just attack the eye,” he added. “It’s in the brain of the horse, and it may be in other organs too. It often starts somewhere else and ends up in the eye. The eye’s the only thing we notice, but horses that have an ERU-affected eye also have inflammation in their brains. We didn’t know that until maybe 20 years ago.”
Brooks confirmed that Appaloosas are at particular risk for moon blindness. “In cases where both of the horse’s eyes are affected, 80 percent of the time it’s an Appaloosa,” he said. “In non-Appaloosas, the rate at which both eyes are affected is only 20 percent.”
The reason isn’t fully understood but seems to be linked to the amount of melanin involved in giving Appaloosas their distinctive coat colors.
“Dogs, cats and humans with little melanin tend to have immune problems with their eyes,” Brooks said. “Melanin is more than just a skin pigment; it’s involved in the eye and in the body’s immune system.”
Solving Treatment Issues
“There are all kinds of therapies [for ERU] as well as non-traditional approaches like acupuncture, because this is such a frustrating disease to treat and people are trying everything they can think of,” Brooks said.
“Various drugs have been tried, including one called cyclosporine A, a drug which interferes with T-lymphocytes,” he added. “Cyclosporine interferes with the body’s immune system. If you have a kidney transplant, you would receive cyclosporine as an anti-rejection drug.”
The challenge, Brooks said, is in getting cyclosporine to the location of the lymphoid follicles, to countermand the over-active immune response.
“You can put [cyclosporine] in an eye-drop or an ointment, but it doesn’t penetrate the cornea very well,” said Brooks. “And giving it orally would be both too expensive, at the dosages needed for horses, and too toxic.”
So veterinarian Brian Gilger, of the North Carolina State University’s Comparative Ophthalmology Research Laboratory in Raleigh, developed a cyclosporine implant.
“He tried various kinds of implants, some of the first ones you had to actually put inside the eye,” said Brooks. “But the one we’re now using, you can insert in the sclera, in the white of the eye.”
Even the most well-behaved horses get tired of eye drops, Brooks said. So as ERU progresses, treatment can become more and more difficult, as the patient starts to fight his handlers. That’s where a cyclosporine implant can be a near miracle. It’s designed to slowly release an effective dosage of the drug, exactly where it can do the most good and keep doing it for up to five years.
“By putting the implant in this position in the sclera, it is close to where these T-lymphocyte follicles are,” Brooks explained. “There, it has the best chance of reducing the intensity of uveitis attacks and of prolonging the intervals between the attacks.
“By itself, the implant is not a cure-all, but it can be very helpful in some horses,” Brooks added. “It’s not going to cure ERU, and it won’t restore the sight which has been lost. But if we can control the condition, then we can preserve the sight the horse has, possibly for the rest of his life.”
ADVERTISEMENT
Brooks said the current style of implant has been in use for about five years, and the results so far are encouraging. Horses who have received the implants have demonstrated no signs of building up a tolerance to the cyclosporine, and if the implant does run out of drug, its silicone composition means it causes next to no irritation and does not need to be removed from the eye. In fact, Brooks believes it would be quite feasible to insert a second implant if necessary.
Surgical Solution
To an owner who has been fighting a losing battle with ERU, surgery may not seem like an extreme solution for an eye condition.
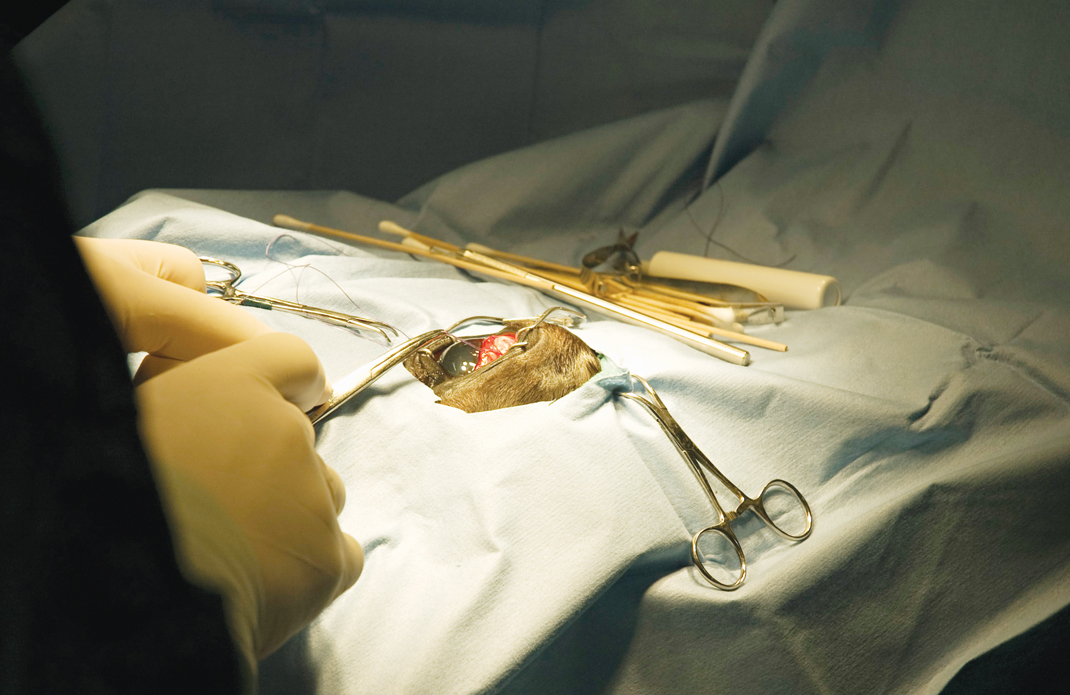
“Most horses [undergoing the implant surgery] are under general anaesthetic for 45 minutes to an hour,” explained Brooks. “It does qualify as microsurgery, and not every veterinary surgeon will want to do it, but it’s not one of the harder techniques.”
Bruce Watt, DVM, a Caledon, Ont.-based veterinarian, consulted with Brooks in order to become one of the first Canadian veterinary surgeons to offer the implants.
“It’s got to go to a very, very exact spot [in the sclera],” said Watt. “You can’t see the implant once it’s in the eye. It’s a little disc about the size of a baby aspirin, but it’s buried under a few layers [of tissue].”
“The results are better if you do the surgery when the disease is controlled,” Brooks added, “but you can do the procedure on a horse who’s experiencing a flare-up. It’s not always possible to get the inflammation controlled, though it does make the surgery easier. The eyes are inflamed anyway, so much so that the sclera can sometimes be twice its normal thickness. These eyes are sick. If you can make the sickness a little bit better, then the surgery has a better chance of success.”
The success rate is impressive. “Eighty percent of the time, a cyclosporine implant reduces the intensity of the attacks in ERU patients, as well as the frequency. Eighty percent is pretty good,” he said.
But, Brooks emphasized, “it won’t eliminate them completely, because anything that’s an immune challenge can trigger a flare-up. Parasites, viruses, anything that triggers an immune system that is too active anyway can start the flare-up. The disease behaves differently in different parts of the world, and veterinarians have to struggle with that because what works in one location may not work in another. The environment plays a big role.”
If necessary, both eyes can be treated in a single surgery, Watt said, and the aftercare is not difficult, usually consisting of antibiotic treatment to fend off infection. The results, however, are not immediately noticeable.
“It takes about a month before the cyclosporine builds up enough in the tissues for it to start working,” said Brooks.
“So you have to continue on the same topical therapy the horse was on before the surgery [until that happens]. The drug is released at a certain specific rate, so it takes a while before the drug is built up to a level which affects those lymphocytes.”
The best candidates for cyclosporine implants are those who have not yet suffered extensive damage or vision loss. Ideally, their ERU should be controllable with topical medications, even if the horse has frequent recurrences. Vision should be good between episodes, there should be minimal scarring or cataract formation, and little to no retinal degeneration or loss of function. Any other active systemic illness, such as a high blood titer for leptospirosis (indicating that disease is still active), might also rule a horse out for the surgery.
“In the best case scenario, we would like to install these implants before too much damage has been done by ERU,” said Brooks. “But we don’t always have that luxury. We want to try to save their sight as long as possible.”
With the cyclosporine implants not yet widely available, this is specialized surgery which is not offered on a routine basis across North America, but if your horse has moon blindness, it’s worth seeking out a veterinary ophthalmologist at your nearest university veterinary college. ERU horses need no longer continue to be blinded by the light.
If you enjoyed this article and would like to read more like it, consider subscribing. “New Hope For Moon Blindness“ ran in the Nov. 19, 2010 issue. Check out the table of contents to see what great stories are in the magazine this week.